Robotic-assisted surgery for colorectal cancer
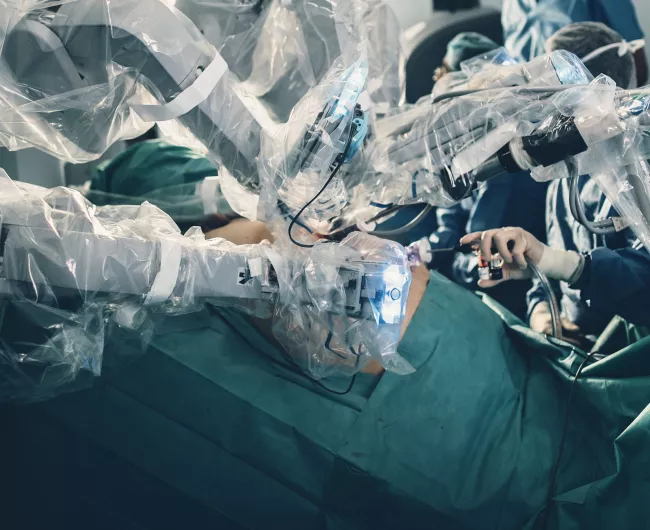
What is robotic-assisted surgery?
Robotic-assisted surgery (also called robotic surgery) is a type of minimally invasive surgery.
Robotic surgery allows doctors to perform complex procedures with more precision, flexibility, and control than is possible with the human hand.
Instead of a large incision, the surgeon makes a few very small incisions (about ¼ to ½ inch) into the abdomen to insert the small “arms” of the robot. A slightly larger incision, about two inches wide, is made to remove the tumor.

Why have robotic-assisted surgery?
Advantages to robotic-assisted surgery are similar to those of laparoscopic surgery.
They include:
- Less recovery time
- Lower risk of infection
- Smaller scars
- Less pain and discomfort after surgery
- Shorter hospital stay
- Speedier return to normal activities

Who is eligible for a robotic-assisted colectomy?
Many colorectal cancer patients are good candidates for robotic-assisted colectomy surgery.
The best option for you depends on several factors, including:
- your overall health
- your medical history
- your surgeon’s experience
- the cancer stage
- the cancer location
What happens during a robotic-assisted surgery?
- During this type of procedure, the surgeon operates a robotic surgical system that has a camera arm and mechanical arms with surgical instruments attached to them.
- The surgeon controls the arms while seated at a computer near the operating table and can see the procedure in a high-definition, magnified, 3-D view.
- Carbon dioxide gas is used to inflate the abdomen and create space for the surgeon to see and operate inside the abdominal cavity.
- The surgeon will remove the segment of the colon or rectum that contains the tumor through the larger incision, along with some lymph nodes.
More about robotic-assisted surgery and colorectal cancer
Learn more about how robotic-assisted surgery is used for colorectal surgery in this helpful video.
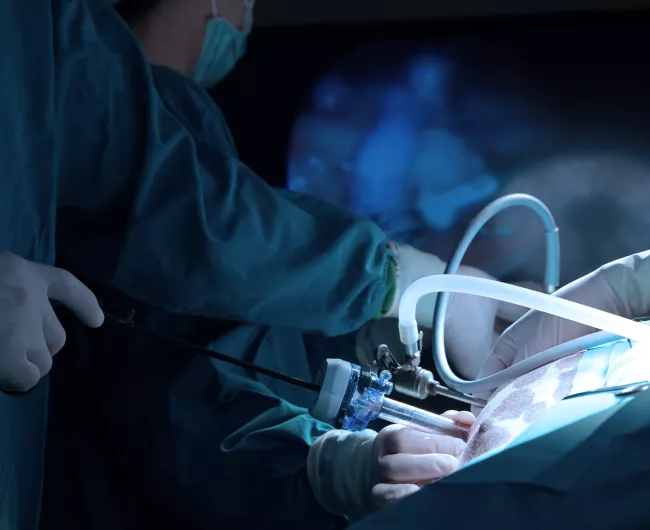
What's the difference between robotic-assisted and laparoscopic surgery?
While these two methods are similar, there are some differences:
Laparoscopic surgery is performed by hand, with the help of a two-dimensional camera.
Robotic-assisted surgery requires the surgeon to operate instruments from outside the patient’s body, using aconsole and a three-dimensional camera.
Related reading
Surgery risks & complicationsTop resources

Christy Williams: Biomarker testing leads to successful treatment
Statistics suggested that Christy’s odds of survival were grim, so she leaned into her faith and kept a positive outlook. She tried to control what she could. And, critically, she received biomarker testing.

EPIC Act to Advance New CRC Therapies Needs Support
The EPIC Act would encourage investment in clinical trials for additional uses of existing drugs.

Michelle Cappel: Biomarker testing extends life
Michelle Cappel owes a lot to colorectal cancer biomarker testing — seven years of life and counting.





