
Managing pain from an ostomy
An ostomy should not cause discomfort. If your ostomy becomes painful, tell your doctor right away.
What causes ostomy pain?
Several conditions can lead to ostomy pain. Common causes include:
- Skin irritation
- Blockages
- Ballooning
- Stoma trauma
- Infection
- Prolapses, retractions, and herniations
How to limit skin irritation
Skin irritation is usually due to a leak from an ostomy device. This can be painful and damaging to your skin and your stoma.
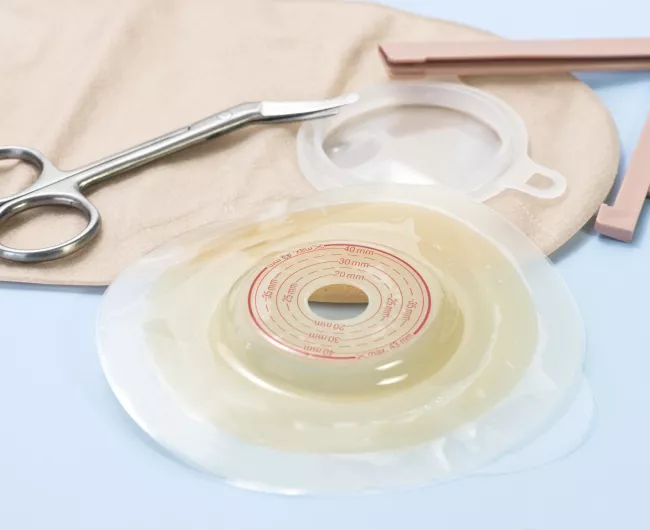
Ensure a good fit
Each time you change a bag, measure the stoma and cut your wafer to the correct size (1/8" bigger than the stoma). This lets the stoma expand without getting suffocated by a wafer that is too tight.
Watch for dermatitis
Contact dermatitis occurs when damaged skin becomes irritated. Allergic dermatitis is a reaction to ostomy products like pouches or barrier rings. Irritant dermatitis is irritated skin from feces or certain products like pastes or solvents. Check with your care team for product options.
Be gentle
Mechanical irritation can cause red, weepy skin around the stoma. It may be caused by washing the skin too aggressively or removing the ostomy device too forcefully. Try holding your skin tight, and gently remove the bag by peeling the adhesive wafer downward.
Drying your skin between bag changes reduces infections
A peristomal fungal infection thrives in dark, moist, and warm environments. Make sure your skin is completely dry before replacing your device. Some people use a hairdryer set to "cool," while covering the stoma with toilet paper.

Avoid blockages
Signs of a blockage include clear output, thin liquid with a strong odor, cramping near the stoma, swelling of the stoma or abdomen, and lighter urine or a decrease in darker urine.
Three steps for managing blockages
An ostomy blockage can happen for many reasons. If you experience one, try these steps.
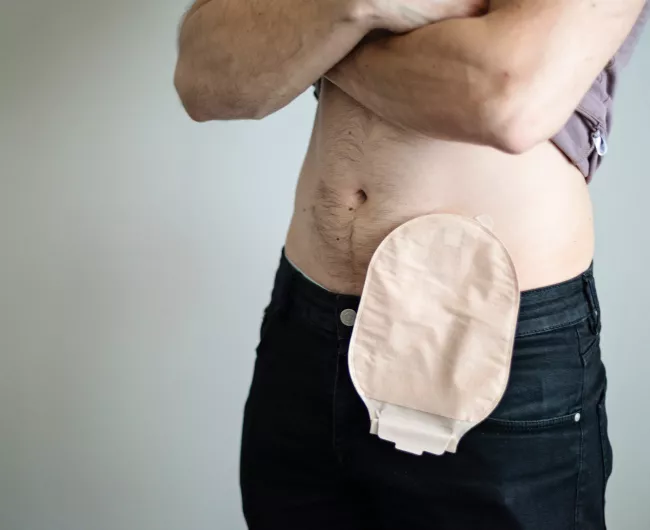
What is ballooning?
Swallowing food or water introduces air into ostomy pouches. Charcoal filters release this air, but if overwhelmed or wet, ballooning may occur. There are ways to limit these uncomfortable effects.
Tips to reduce ballooning
Take your time
Eat and drink slowly, trying not to hurry or rush while doing so. Make sure to chew your food completely.
Try probiotics
Adding daily probiotics to your routine balances the bacteria in your system, which can help diminish gas.
Avoid certain activities
Drinking through a straw or sports cap bottle, chewing gum, smoking, and snoring may increase swallowed air.
"Burp" your one-piece bag
Tilt the bag up to prevent spilling and slowly guide the air through your bag to the drain/spout. Do this in a well-ventilated area.
"Burp" your two-piece bag
Partially unclip the wafer from the bag at the very top and gently push out the excess air. Do this in a well-ventilated area.
Call the Helpline
Our Helpline is free. Connect with certified patient and family support navigators who are ready to listen and support you.
Top resources
Kat Sisler: From ostomy-opposed to ostomy-grateful
My cancer and ostomy journey began with a rude awakening in January 2023. My father was diagnosed with colorectal cancer at 42, and given that history, I asked my doctor at my yearly physical when I should begin screening.

Empowering lives: celebrating World Ostomy Day
Every year on the first Saturday of October, people worldwide come together to celebrate World Ostomy Day, also known as Ostomy Awareness Day. This day serves as a reminder of the resilience, strength, and courage millions of individuals display each year living with an ostomy.
How to cut and fit an ostomy wafer for a stoma
In this video, ostomate and certified patient and family support navigator Stephanie Rouse demonstrates how to cut and fit an ostomy wafer, or skin barrier, for a stoma.





